
Dr Alasdair Munro is a Clinical Research Fellow in Paediatric Infectious Diseases at the South Hampton Clinical Research Facility. He is the review lead at the incredibly helpful Don’t Forget the Bubbles website which summarises the epidemiological evidence on COVID-19 as it comes out, especially as it relates to children. I have found their reviews to be the most up to date and helpful of the many that are popping up on the web. Yesterday Dr Munro went through a list of current questions people have on children and COVID-19 and posted their latest thinking on the research informing their views on children and COVID-19. I’m re-blogging that here because I found it so helpful!
Dr Munro: “With so much attention on COVID19 in children, it’s time for an updated Tweetorial on what we do and don’t know. We’ll talk impact, risk, hyperinflammation syndrome, transmission, schools and more. Firstly, children remain grossly underrepresented in all case numbers, hospital admissions and deaths worldwide. See the latest ISARIC report of more than 15,000 severe cases, or Public Health England UK deaths.
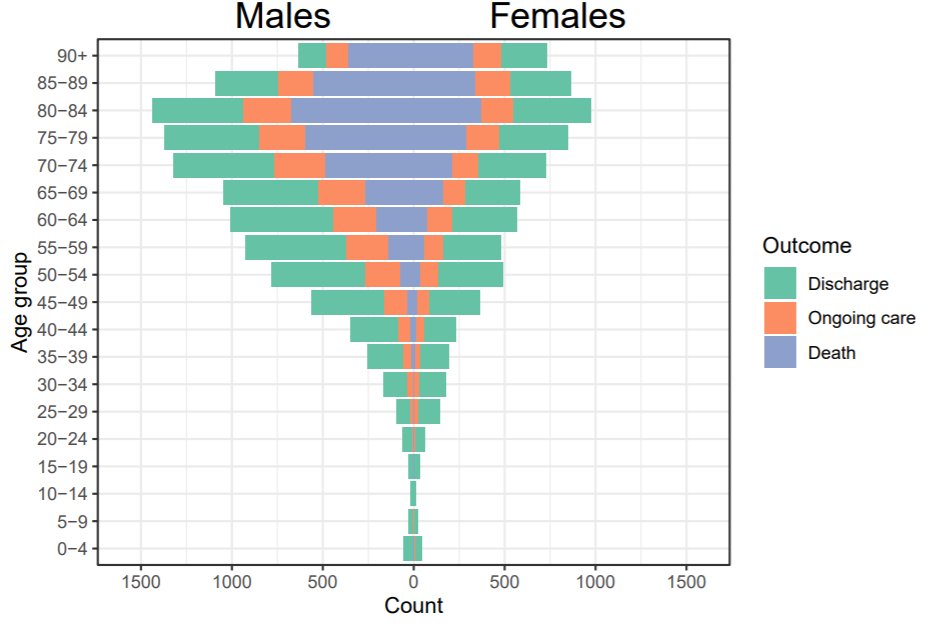
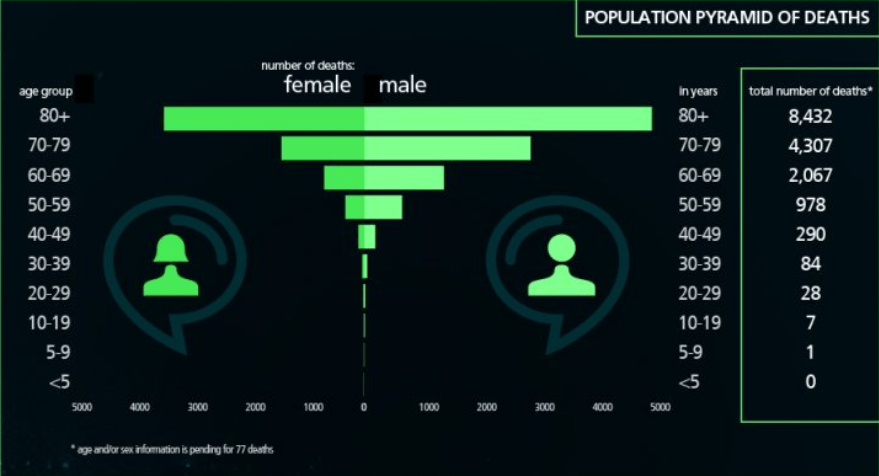
This report from Prof Sunil Bhopal and friends looks at child deaths from COVID19 compared to other causes to put them in perspective. Of about 37,000 child deaths, 43 were from COVID19. In the words of Prof David Spiegelhalter, children are “unbelievably low risk”
Are some children higher risk? Small numbers, but children usually at risk from viral respiratory infections look equally at risk from #COVID19, including tech dependent, neurodisability, malignancy or chronic lung disease (see here and here). Important to note that outcomes are still pretty good for these groups, and there are a number of documented cases for some (e.g. oncology, immuno-suppressed) which had a predominantly mild clinical course. Even most of these children don’t get very sick. What about this hyper inflammatory syndrome? It’s called PIMS-TS (or MIS-C in the USA). It seems to be an immune reaction after COVID19 infection (approximately 2 – 4 weeks after). It usually starts with persistent fever, abdominal pain and diarrhoea and vomiting, then can present similar to Kawasaki Syndrome (+/- shock).
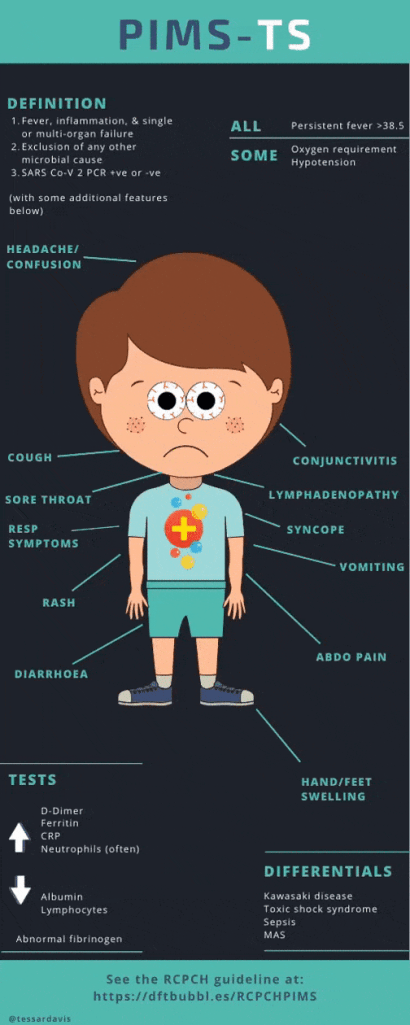
We currently have 3 published cohorts from London, Italy and France. Many kids get very sick, but most recover well. It seems to be dissipating (following trends in peaks of infection). Read more about it here. It can be serious, but is incredibly rare. In Europe there have been about 230 cases and very few deaths. There are more than 80-million children and the European Centre for Disease Control (CDC) considers it a low risk. Be reassured.
OK what about transmission? Let’s go step by step. How easily do children catch it? Five studies have looked at transmission to children (mainly household) and 4 out of 5 found significantly lower attack rates in children than adults.
How many children actually have or had COVID19? Well, less than 2% of known cases have been in children, but given symptoms are so mild have we just missed them all? Are they mainly asymptomatic? Are they silent assassins? This is harder to tell, but there is some evidence. Iceland tested those at risk and found half the rate of infection in children under 10 years compared to adults, and zero cases in asymptomatic screening. Vo, Italy screened more than 85% of their population and 2.6% had COVID19, but no children under the age of 10.
Some say the UK Office of National Statistics data shows there’s no difference between children and adult infection rates. But they found about 30 positive cases in 10,000 people. The confidence intervals are too wide for inference about relative infection rates (compatible with 10x rates in any group).
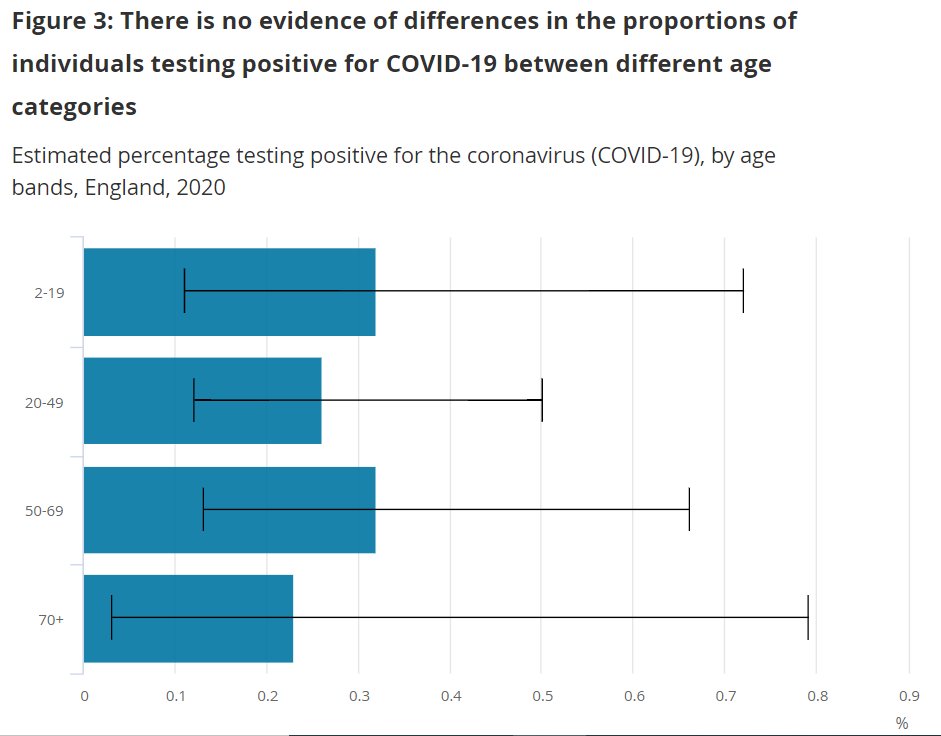
The same principle applies for 2 sero-epidemiological studies from Switzerland & Germany. Despite lower rates of infection in children, numbers are too small to be statistically significant. This is not evidence for equal rates of infection.
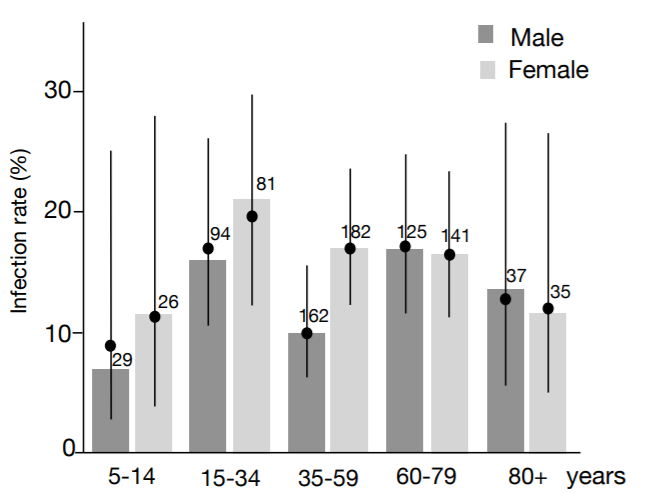
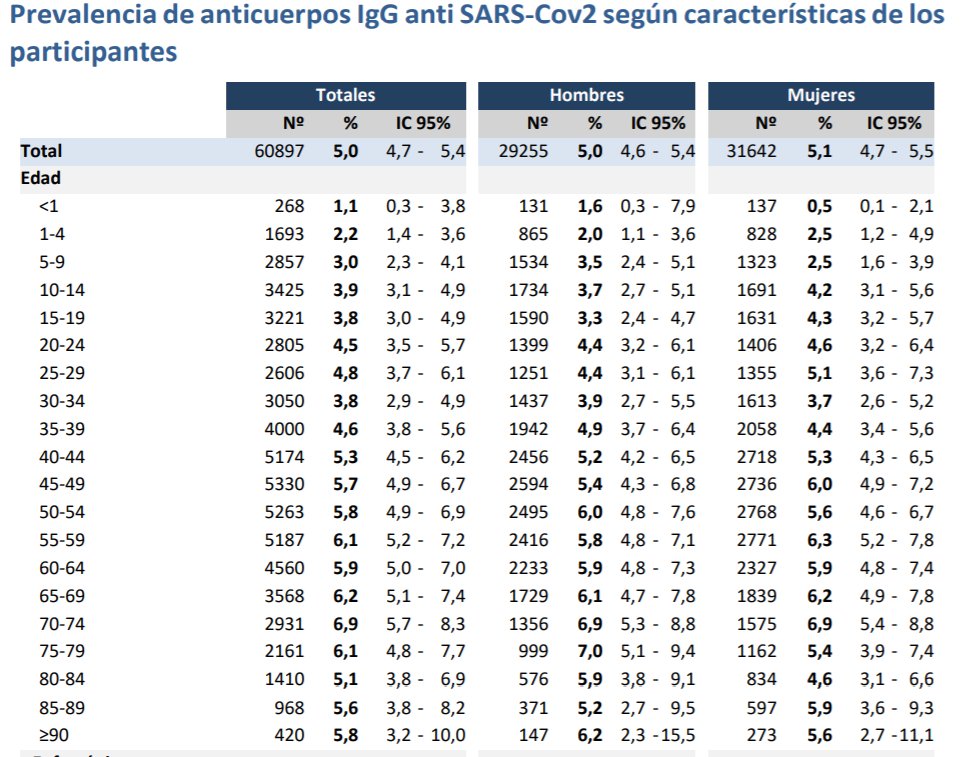
What do we find if we do a proper sized sero-epidemiological study? Infection rates of 1-3% in children compared to 5% in adults in a Spanish study of more than 60,000 people.
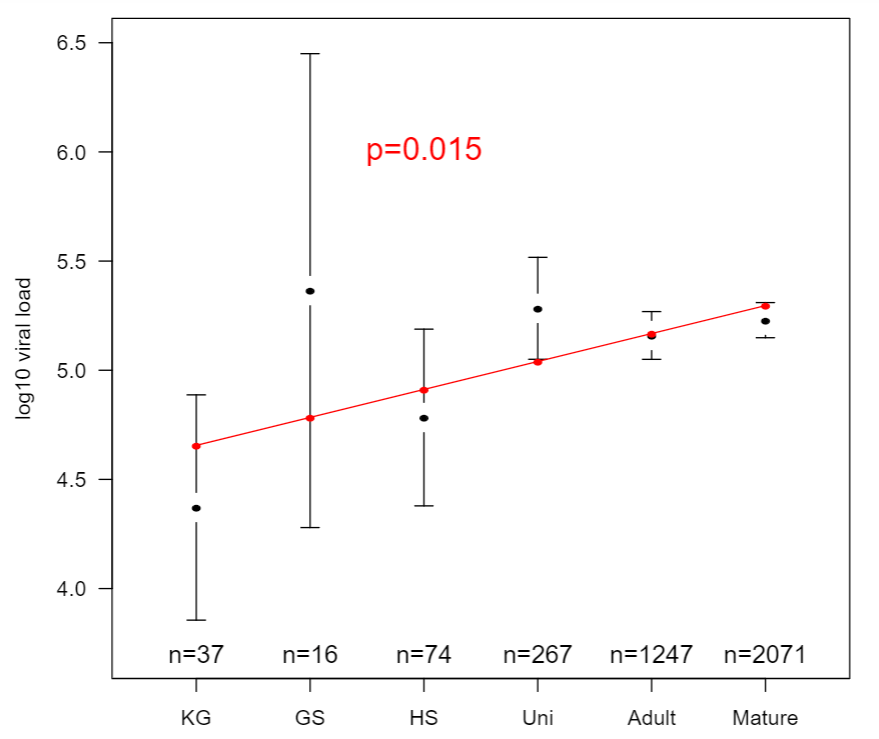
How infectious are children when infected? Hard to say. Some examples of children not spreading at all despite multiple exposures (more than 100 other children) but spreading other respiratory viruses. A German study claimed to find similar viral loads in children as adults, stating they’re “just as infectious.” Amongst other issues, if analysed properly the data actually showed significantly lower viral loads in children.
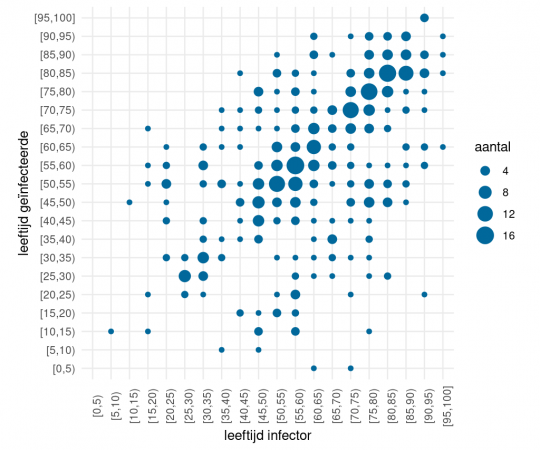
National reports from the Netherlands, Iceland, Norway, Australia have found limited evidence of children contributing to spread of COVID19. Most transmission is adult to adult.

What does it mean for schools? Children can get COVID19 so they can almost certainly spread it. But, they are barely affected by infection, and appear less likely to catch or spread it than adults (see here). Schools seem lower risk than adult work environments. Will outbreaks happen? Of course. But this is our new reality for the foreseeable future. We need to mitigate against the risks and ensure mechanisms for quick response (track, trace and isolate) are in place. Children suffer harm from lockdown (see here).
Now for why children seem so much less affected… Still no clear answers. Possible differences in ACE2 expression, but they seem small. Some suggest immune differences. This needs to be proven. More research needed!
Thanks for making it to the end! For our comprehensive review of all paediatric #COVID19 literature (cited by UK Research and Innovation and World Health Organisation) check it out here on Don’t Forget the Bubbles.
Follow Dr Alasdair Munro on Twitter at @apsmunro


